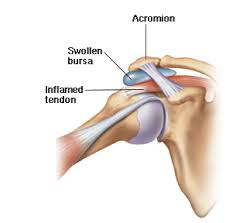
When people experience shoulder pain, whether acute or chronic, they often become fearful of the infamous rotator cuff tear. While rotator cuff tears are a significant injury, and something to be concerned about, they make up only a small potion of all shoulder complaints. More often than not, the person’s shoulder pain, and often resultant neck pain, can be contributed to what is known as Shoulder Impingement Syndrome. As the name implies, the soft tissues of the shoulder often become impinged upon/compressed secondary to repetitive stress, muscle weakness, muscle tightness, and poor posture. These soft tissues include muscle tendons, such as the biceps and supraspinatus (smallest, upper-most rotator cuff muscle), and the sub-acromial bursa ( a small sac of connective tissue/fluid that acts as a shock absorber for the shoulder/collar bone). Over time, this repetitive impingement leads to inflammation of the tendons and bursa, resulting in tendinitis and bursitis, respectively. Pain associated with impingement syndrome often develops gradually over a period of time, with the primary focus being towards the front and side of the shoulder joint. If left untreated, the repetitive irritation may result in fraying and tearing of the underlying tendons (now we have our more serious rotator cuff tear).
In a typical healthy shoulder the supraspinatus muscle is able to glide freely in an opening between the shoulder blade and collar bone, just beneath the AC-joint. However, this space is often compromised and becomes more narrow with repetitive activities involving over head or inward movements of the shoulder and arm. These activities may include, but are not limited to, swimming, throwing, painting, overhead sports, lifting, sleeping on your stomach, excessive computer use, and extended driving. The shape of your collar bone, or the development of arthritic bone spurs, in specific locations, are also important factors in developing impingement syndrome. While x-rays may be useful in identifying these risk factors, they are typically unnecessary in diagnosing impingement syndrome; your Doctor of Chiropractic can often make this diagnosis based on history and physical examination alone.
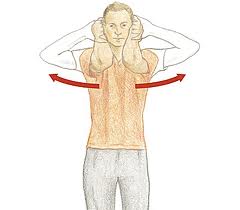
When treating impingement syndrome, or any musculoskeletal injury for that matter, it is important to exhaust all conservative options prior to moving forward with more invasive procedures. As the shoulder becomes inflamed your body undergoes a compensation process, trying to avoid the pain, in which certain muscles become weak while others go into spasm. This imbalance further creates aberrant motion of the shoulder joint, shoulder blade, mid-back, and neck. The first goal of conservative care is to reduce the pain and inflammation, while simultaneously improving range of motion. This can be accomplished in various methods, including chiropractic adjustments, soft tissue work (including myofascial release and instrument assisted soft tissue mobilization), nutritional support, and focused exercises and stretches. The main focus of the stretches/exercises should be to avoid aggravating postures in which the shoulders and mid-back round forward, further restricting normal shoulder movements.
As a rule of thumb, the longer an injury takes to develop, the longer it takes for the injury to recover; this also holds true for the individual who simply ignores the pain in hopes that it will clear up on its own. With this being said, while you cannot expect to fully recover in a matter of days, or weeks, you should see some signs of improvement (e.g. pain reduction, improved range of motion, no longer pain putting on jacket, etc.). If symptoms persist, despite being treated, your Doctor of Chiropractic may consider referring you for an MRI (to assess for underlying tears), pain management (e.g. pain creams or corticosteroid injections), or to see an orthopedic surgeon. More invasive forms of treatment, such as cortisone injections, should be reserved for cases that are non-responsive, or extremely painful. While these injections are effective at reducing inflammation, they do not address the underlying dysfunction responsible for causing the impingement, and carry with them their own set of inherent risks.